ZIKA VIRUS
Luciano Schiazza M.D.
Dermatologist
c/o InMedica - Centro Medico Polispecialistico
Largo XII Ottobre 62
cell 335.655.97.70 - office 010 5701818
www.lucianoschiazza.it

Zika fever is an illness caused by the Zika virus a member of the Flaviridae family.
It is spread to people through the bite of mosquitos from the Aedes genus ( Aedes aegypti, Aedes africanus, Aedes apicoargenteus, Aedes furcifer, Aedes hensili, Aedes luteocephalus and Aedes vitattus), primarily Aedes aegypti in tropical regions and Aedes albopictus in more temperate. Aedes are the same mosquitos that spread dengue and chikungunya. During the 2007 outbreak on Yap Island in the South Pacific, Aedes hensilli was the vector, while Aedes polynesiensis spread the virus in French Polynesia in 2013.


The first known case of Zika fever was isolated in 1947 from a rhesus macaque in the Zika forest (a relatively small forest) of Uganda, Africa in 1947 (zika means “overgrown” in the Luganda language). The Zika forest acts as a virus research field station for the East African Virus Reasearch Institute in Entebbe, Uganda.
The monkey developed a fever, and researchers isolated from its serum a transmissible agent that was first described as Zika virus in 1952. The first human cases were reported in Nigeria in 1954.
The pathogenesis of the virus is hypothesized to first infect dendritic cells near the site of inoculation, and then spread to lymph nodes and the bloodstream. In terms of replication, flaviviruses generally replicate in the cytoplasm, but Zika virus antigens have been found in infected cell nuclei.
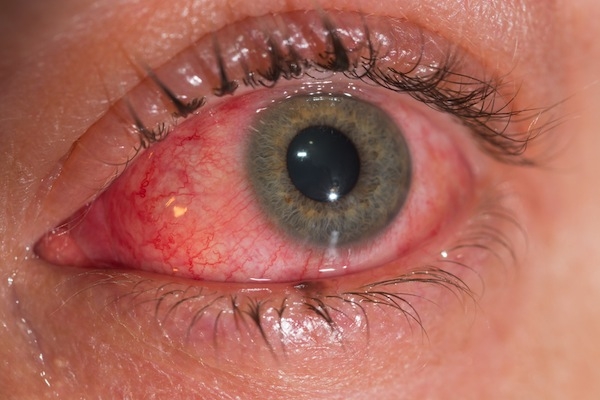
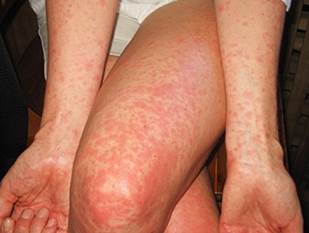
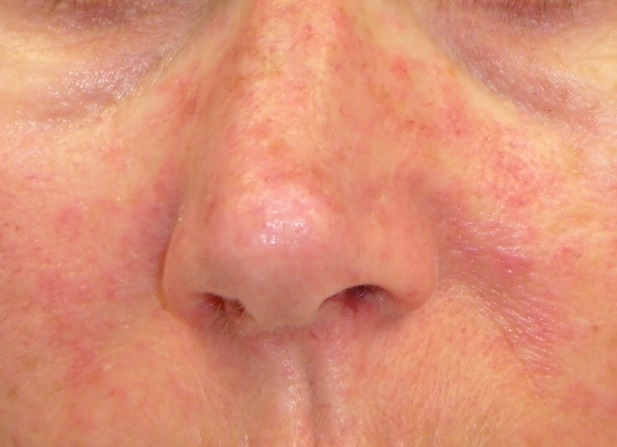
Symptoms are similar to other flaviviruses. The majority of cases (60-80%) are asymptomatic. The main clinical symptoms in patients begin with a low-grade fever (37,8°C e 38,5°C), mild headache, non purulent conjuntivitis, transient arthritis/ arthralgia (mainly in the smaller joints of the hands and feet) and maculopapular rash that often starts on the face and then spreads throughout the body.
In general the disease is short-lasting (2–7 days).
From its discovery until 2007, confirmed cases of Zika virus infection from Africa and Southeast Asia were rare. In 2007, Zika virus caused a major epidemic (with 185 confirmed cases) on the island of Yap, Federated States of Micronesia, in the Pacific. This was the first documented transmission outside of its traditional endemic areas in Africa and Asia. The mosquito Aedes hensilli, was the predominant species identified in Yap during the outbreak, and probably the main vector of transmission.
More recently (2013), epidemics have occurred in Polynesia, Easter Island, the Cook Islands and New Caledonia.
In May 2015, Brasil officially reported its first 16 cases of the illness.
| Countries reporting local transmission of confirmed Zika virus infections in past nine months, as of 21 Dec 2015 | ||||
|---|---|---|---|---|
| Brazil | El Salavador | Honduras | Panama | Solomon Islands |
| Cape Verde | Fiji | Martinique | Paraguay | Suriname |
| Colombia | French Guiana | Mexico | Samoa | Vanuatu |
| Guatemala | New Caledonia | Venezuela | ||
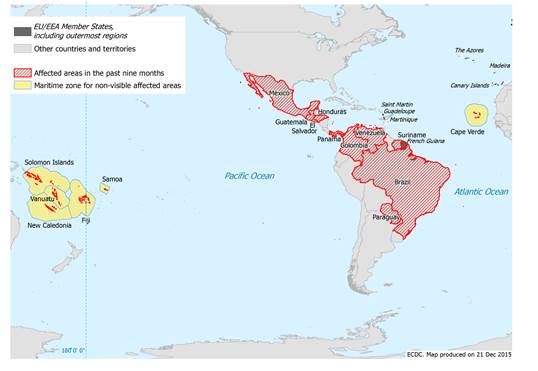
Mosquito-borne Zika virus is suspected to be the cause of 2,400 cases of microcephaly and 29 infant deaths in Brazil in 2015. Detection of Zika virus RNA in human amniotic fluid indicates that the virus can cross the placental barrier, suggesting that fetal infection is possible.
It has been confirmed that Zika virus can be sexually transmitted between humans.
Like other flaviviruses it could potentially be transmitted by blood transfusion.
Zika virus is considered an emerging pathogen with the potential to spread to new areas where the Aedes mosquito vector is present.
Zika virus can be diagnosed by performing RT-PCR test (reverse transcriptase-polymerase chain reaction) in acutely ill patients. The test has been done on serum collected within 1 to 3 days of symptoms onset or on saliva or urine samples collected during the first 3 to 5 days, because the period of viremia can be short. Toward the end of the first week of illness, infection is detected through serologic detection of virus-specific IgM and IgG antibodies. Serological cross-reactions with primary flavivirus infections (such as dengue) as vaccines to flaviviruses are possible, so plaque-reduction neutralization testing (PRNT) can be performed to measure virus-specific neutralizing antibodies.
Differential diagnosis of suspected Zika virus infection include:
dengue, leptospitosis, malaria, rickettsia, group A streptococcus, rubella, measles, parvovirus, enterovirus, adenovirus, alphavirus infections (w.g. Chikungunya, Mayaro, Ross River, Barmash forest, O’nyong-nyong and Sindbis viruses).
There is no vaccine and treatment is supportive:
-
rest
-
drink fluid to prevent dehydration
-
acetominophen or paracetamol to relieve fever and pain,
-
aspirin and non-steroidal anti-inflammatory drugs (NSAIDs) only when dengue has been ruled out.
-
aspirin use is generally avoided in children because of the risk of Reye syndrome.
About prevention, because the virus is spread by mosquitoes, vector control and avoidance are essential elements to disease control.
Individuals that can be exposed to mosquitos are recommendedto:
-
Cover exposed skin (long-sleeved shirts and long pants),
-
Use insect repellent,
-
Stay and sleep in screened-in or air-conditioned rooms,
-
Use permethrin-treated clothing and gear (such as boots, pants, socks, and tents)
-
Use a bed net if the sleeping room is exposed to the outdoors.
