AQUAGENIC WRINKLING OF THE PALMS
Luciano Schiazza M.D.
Dermatologist
c/o InMedica - Centro Medico Polispecialistico
Largo XII Ottobre 62
cell 335.655.97.70 - office 010 5701818
www.lucianoschiazza.it
Wrinkling of the palmar and plantar skin is a normal response to prolonged water immersion occurring on average 11.5 minutes after exposure to water. Aquagenic wrinkling of the palms (AWP) is an excessive, exaggerate, strong wrinkling of the palms that appears shortly after immersion in water (the so-called “hand in bucket sign”).
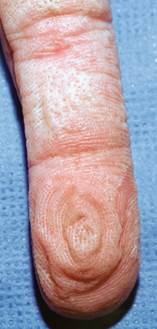
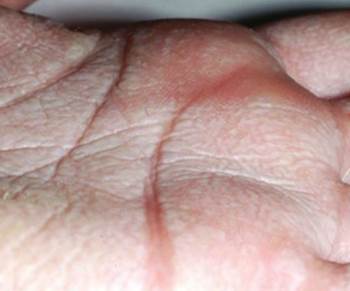
It is characterized by a rapidly development of small, flesh-colored to white, translucent edematous, flat-topped papules with dilated ostia on the palms and finger margins (restricted to the glabrous skin). These changes may be asymptomatic or associated with discomfort (pruritus, pain, burning, tingling, numbness, tightness) and functional impairment.
The skin lesions usually disappear soon after being dried but sometimes can persist for a few hours or longer periods. When not exposed to water, the skin of affected patients usually looks normal.
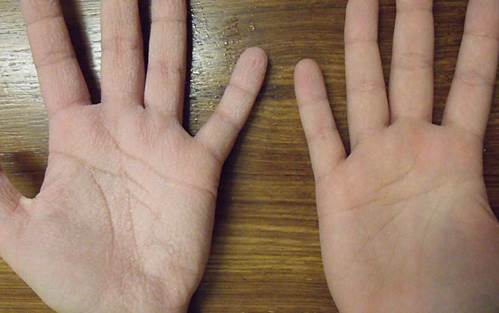
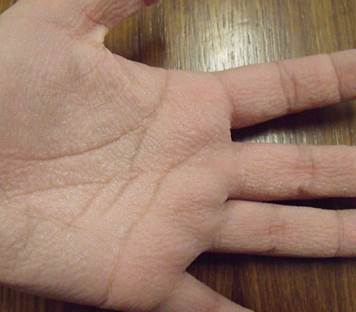
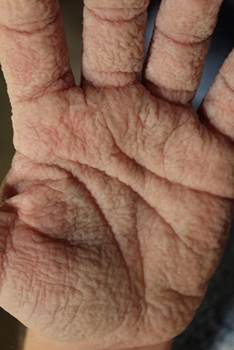
Aquagenic wrinkling of the palms (AWP) often occurs in patients with cystic fibrosis but it may also occur in carriers of the cystic fibrosis gene Symptoms appeared after a few minutes (usually less than 2 min) after exposure to both warm and cold water (“hand in the bucket sign”), particularly after showering and washing dishes.
It was worse with warm weather, and was triggered also by perspiration and gloves. The symptoms did not occur in sea water.
Moreover, plantar involvement was not commonly observed Aquagenic wrinkling of the palms was first reported in 1974 by Elliot in a 1-paragraph letter to the Lancet entitled “wrinkling of skin in cystic fibrosis” in which he described an anecdotal observation in children with cystic fibrosis (CF), suggesting that “three minutes and a bowl of water might provide a cheap screening test [for CF].”
Several, different names have been used in the literature describing a morphologically similar, yet distinct condition:
-
transient reactive papulotranslucent acrokeratoderma,
-
aquagenic syringeal acrokeratoderma,
-
aquagenic palmoplantar keratoderma,
-
acquired aquagenic palmoplantar keratoderma, ,
-
aquagenic keratoderma,
-
wrinkling of skin,
-
transient aquagenic palmar hyperwrinkling,
-
early aquagenic wrinkling.
The cause of AWP is unknown but it has been postulated to be a result of a salt imbalance in the skin cells due to an abnormal electrolyte fluxes that result in sodium retention within epidermal keratinocytes with increased water retention within these cells and increased transepidermal water loss. In CF there is , loss of functional CF transmembrane conductance regulator (CFTR) results in reduced electrolyte reabsorption in the eccrine ducts and, thus, hypertonic sweat. This hypertonicity may lead to an increased rate of diffusion of water into the palmar skin and hence AWP.
Alternatively, CFTR abnormalities may afflict flux of water into the skin via a different mechanism. CFTR has been shown to activate aquaporins and aberrant aquaporin 5 expression has been demonstrated in the sweat glands in AWP. AWP can also be drug-induced (cyclooxygenase COX-2 inhibitors like rofecoxib, aminoglycoside, aspirin).
The proposed mechanisms for these cases involve an increased sodium reabsorption in a mechanism similar to the effect of COX-2 inhibitors on kidney cells. Alternative hypotheses for the pathogenesis of AWP have implicated a defective barrier function of the stratum corneum, occlusion of eccrine duct ostia, weaknesses of the eccrine duct wall, and influx of water across an osmotic gradient into eccrine ducts, eccrine gland or nerve dysfunction, hyperhidrosis, defective barrier function of the stratum corneum, occlusion of eccrine duct ostia and weakness of the eccrine duct wall.
Because patients presenting with AWP, including apprently healthy patients, have an increased risk of having CF or the CF carrier state and because patients with mild forms of CF may develop late.onset or slowly progressive lung disease, identifying these patients and respiratory referral and interventions are important to minimized future morbidity.
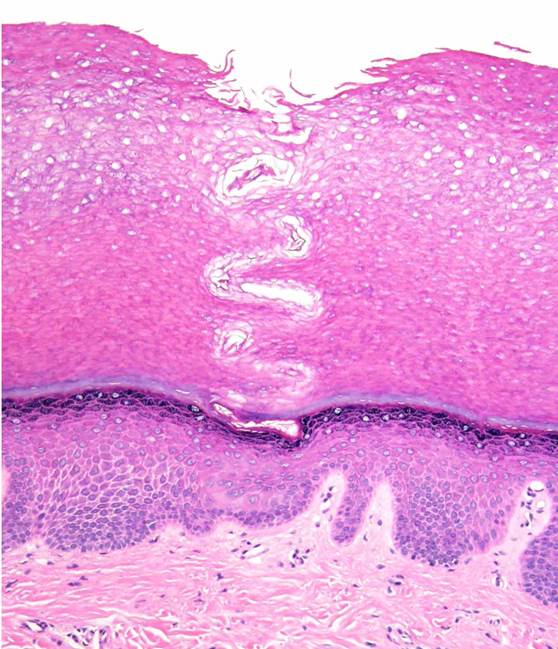
Histologically, hyperkeratosis, dilated eccrine ostia, and aberrant aquaporin-5 expression10 are characteristic.