BULLOUS IMPETIGO
Luciano Schiazza M.D.
Dermatologist
c/o InMedica - Centro Medico Polispecialistico
Largo XII Ottobre 62
cell 335.655.97.70 - office 010 5701818
www.lucianoschiazza.it
Impetigo is an acute, highly communicable, contagious gram-positive bacterial infection of the superficial layers of the skin. Impetigo is caused by Streptococcus pyogenes and Staphylococcus aureus.
The name derives from the Latin impetere (to assail). Exists in two distinct forms:
- nonbullous impetigo
- bullous impetigo
The nonbullous impetigo (impetigo contagiosa), is the more common form. It tends to affect skin on the face or extremities that has been disrupted by minor trauma, such as insect bites, cuts, abrasions, thermal burns, or diseases such as dermatophytosis varicella, herpes simplex, scabies, pediculosi.
It is usually caused by either S. aureus and/or group A β-hemolytic streptococci.
Lesions start, generally around the mouth and nose, as vesicles that quickly rupture, leaving a thick yellowish-brownish golden (honey-colored) crust. Exposed areas, such as the face and limbs, are commonly affected. It heals without any scarring.
The sores are not painful but they itch a great deal: touching or scratching help lesions to spread to other parts of the body and other people. The bullous impetigo unlike nonbullous impetigo, occurs on intact skin skin of intertriginous areas such as the neck, the axillary and crural folds, and the diaper area, but it may appear on the face or anywhere on the body.
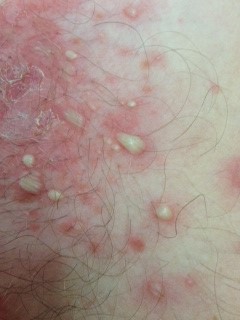
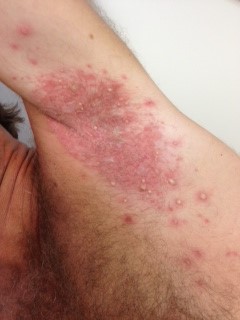
It is secondary to Staphylococcus aureus (primarily phage II, group 71) which produces exotoxins termed exfoliatins. These exotoxins attack a protein that keep skin cells bound together (desmoglein I), cause a loss of intracellular adhesion between keratinocytes, inducing intraepidermal clefts between the stratum corneum and stratum spinosum resulting in vesicles located above the basal cell.
There are some strains of the Staphilococcus aureus that have developed resistance (it means that they are resistant to the medication) to beta-lactam antibiotics, such as the penicillins (methicillin, dicloxacin, nafticillin, oxacillin, etc) and the cephalosporins: these strains are called “methicillin-resistant Staphylococcus aureus” (MRSA).
Lesions of bullous impetigo are vesicles that rapidly progress to small or large (usually less than 3 cm), superficial, thin-roofed, flaccid, and transparent bullae. The bullae initially contain a clear, yellow fluid that subsequently turns cloudy and dark yellow. Bullae rupture easily, within 1-3 days, leaving a rim of scale around an erythematous moist base.
After desiccation, the lesion has a brown-lacquered or scalded-skin appearance, with a collarette of scale or a tubelike rim at the periphery. Intact bullae are not usually present because they are very fragile.
The intact bullae rupture after 2 to 3 days, forming light brown crusts at the borders of erythematous erosions. The lesions usually spread locally and may rich distal areas through direct autoinoculation.
Fever, diarrhea, generalized weakness may be present in bullous impetigo. S. aureus colonizes (colonization means presence of bacteria on a body surface without causing infection) in the anterior nares (the nostrils) in approximately 30% of individuals, 10% in the perineum and, more uncommonly, in the axillae, pharynx, and hands.
Some people are permanent carriers and reservoirs of the infection for other people. Bacteria can spread from the nose or other sides colonized, to healthy skin within 7-14 days, with impetigo lesions appearing 7-14 days later.
Bullous impetigo heals without scarring. Bullous impetigo can affect people of all races and of all ages but is most common in children 2-5 years of age.
The incidence in males and in females are equal but in adults, however, impetigo is more common in men. The prevalence of impetigo varies seasonally, with peak incidence during summer and fall; but seasonality may not occur in regions that remain warm and humid throughout the year.
Bullous impetigo is considered to be less contagious than nonbullous impetigo. Contributory or predisposing factors for bullous impetigo are:
- hot, humid weather or environment,
- minor trauma,
- participation in contact sports,
- overcrowded living conditions,
- pediatric settings, including hospital nurseries
- poor personal hygiene,
- colonization of nares, axillae, perineum,
- an unhygienic work environment
- skin contact in locker rooms and gyms
Conditions such as HIV infection, posttransplantation, diabetes mellitus, hemodialysis, chemotherapy, radiation therapy, or systemic corticosteroid treatment increase susceptibility. Diagnosis of impetigo is generally based on history and clinical appearance. But, occasionally, other conditions may look something like impetigo. So alternative diagnostic possibilities are key to consider, especially in recurrent cases or in those that do not respond quickly to treatment:
- dermatophitic infection (“ringworm”)
- herpes cold sores (herpetic impetigo)
- poison ivy
- bullous pemphigoid reaction
- folliculitis (superficial hair follicle infection)
- pseudomonas folliculitis
- follicular mucinosis
- cutaneous candidiasis
- bullous lupus erythematosus
- bullous scabies (mites)
- sweet syndrome (acute febrile neutrophilic dermatosis)
- linear immunoglobulin A bullous dermatosis
- dermatitis herpetiformis
- bullous-fixed drug reaction
Impetigo is not serious and is very treatable. The aim of treatment is to speed up healing, improve the skin's appearance and prevent complications and the spread of infection. Treatment will depend on the type of impetigo and the severity of symptoms and typically involves local wound care along with antibiotic therapy, with a topical agent alone or a combination of systemic and topical agents. Affected skin can be handled by gentle cleansing, washing affected areas with warm, soapy water.
Topical antibiotic therapy
is considered the treatment of choice for individuals with uncomplicated localized impetigo. Topical therapy eradicates isolated disease and limits the individual-to-individual spread. If possible, it would be better to use latex gloves applying the cream. Afterwards hands should be washed thoroughly. Topical antibiotics commonly used are:
- Mupirocin is a naturally occurring antibiotic produced by fermentation of Pseudomonas fluorescens. The mechanism of action of mupirocin is via inhibition of bacterial protein synthesis. Mupirocin topically is used three times daily usually for up to 10 days. Labeled for ages three months and older
- Retapamulin is a topical antibiotic available as a 1% ointment. It is the first of a new antibiotic class called pleuromutilins. This agent doesn’t directly kill the bacteria but works by preventing bacteria from producing proteins that are essential to their growing and replicating (inhibition of protein synthesis by binding to the 50S subunit on the ribosome). It should be applied only to small areas of skin. Twice a day for five days. Labeled for ages nine months and older.
- Fusidic acid is an antibiotic derived from the fungus Fusidium coccineum. Itinhibits bacterial replication (protein synthesis inhibition) and does not kill the bacteria but stops bacteria from reproducing (bacteriostatic). It should be applied to the infected area two or three times a day.
- Hydrogen peroxide 1% cream is a bleach that when applied to tissues releases oxygen (oxidising agent) with actericidal activity. The cream has to be applied 2-3 times daily on the affected skin area.
When the impetigo is more widespread or if the patient has not responded to topical antibiotics or skin lesions are associated with systemic manifestations, a course of systemic antibiotics that have gram-positive bacterial coverage is indicated.
Beta-lactamase resistant antibiotics (eg, cephalosporins, amoxicillin-clavulanate, cloxacillin, dicloxacillin) are recommended. Cephalexin appears to be the drug of choice for oral antimicrobial therapy in children. Erythromycin and clindamycin are alternatives in patients with penicillin hypersensitivity.
If MRSA is suspected, alternative antibiotics include clindamycin, trimethoprim-sulfamethoxazole, and vancomycin.
The patient should respond to treatment within seven days. It is important to complete the course, even if symptoms clear up early.
For patients with recurrent impetigo, asymptomatic family members, and S aureus nasal carriers, it is important to prescribe 2% mupirocin cream or ointment (Bactroban) for application inside nostrils 3 times per day for 5 days each month to reduce colonization in the nose.
A follow-up visit within 1 week is important to ensure complete clearing of lesions. If impetigo has not improved, a bacterial culture has to perform looking for the sensitivity results, prescribing antibiotic accordingly.
Methicillin-resistant Staphylococcus aureus (MRSA) should be suspected in cases of spontaneous abscess or cellulitis and in lesions that do not resolve with traditional antimicrobial therapy.
It is important a good personal hygiene such as keep nails short to reduce scratching and clean and wash hands as indicated by World Health Organization.
To determine whether a patient is an S aureus carrier, a bacterial culture of the nares may be obtained. If the nares culture is negative and the patient has persistent recurrent episodes of impetigo, bacterial cultures should be obtained from the axillae, pharynx, and perineum. In cases of recurrent impetigo in patients with negative S aureus carrier status and no predisposing factors such as a preexisting dermatosis, is necessary obtain serum immunoglobulin M (IgM) levels to rule out primary selective IgM deficiency.
But frequent association of IgA, IgG deficiencies have also been reported. Because of the contagious nature, children with impetigo should avoid close contact with other children and should not return to day care or school until 24 hours after the initiation of appropriate antimicrobial therapy.
About prevention of impetigo, good hygiene is the best way to reduce the risk of developing or spreading impetigo. Cuts, scrapes, grazes, and insect bites should be washed immediately and kept clean. If somebody has impetigo it is important to keep their belongings (fomites including clothing and toys) isolated from other people and must not be shared or worn by other people. The patient's clothes, bedding, towels and other toiletries should be washed daily.
It is important to inspect household members for impetiginous lesions because failure to treat other infected persons may result in continued transmission.
To prevent a recurrence of impetigo, treat properly any skin condition, such as eczema.
